Diabetic Retinopathy: Symptoms, Causes and Treatments
The Importance of Managing Diabetes and Preventing Blindness
What is Diabetic Retinopathy?
Globally, diabetic retinopathy is the leading cause of vision loss and preventable blindness in working-age adults (20–65 years). https://www.aaojournal.org/article/S0161-6420(21)00321-3/abstract
145 million people have diabetes, as of 2015.
Diabetic retinopathy is a condition that results in microvascular manifestations in the retina of the eye. As a complication of Type 1 diabetes mellitus (DM) and Type 2 diabetes, diabetic retinopathy results from high blood glucose level levels and dysregulation of the body's glucose pathways.
Because diabetes rates are on the rise, so too are the rates of diabetic retinopathy. Diabetes affected 415 million people in 2015 https://www.aaojournal.org/article/S0161-6420(21)00321-3/abstract and is estimated to almost double to 700 million in 2045. https://www.thelancet.com/journals/landig/article/PIIS2589-7500(20)30250-8/fulltext Approximately one-third of people with diabetes develop some form of diabetic retinopathy. https://eyesurgeryguide.org/understanding-diabetic-retinopathy-key-data-and-statistics/ Vision loss due to diabetes can be due to a multitude of reasons besides diabetic retinopathy, including diabetic macular edema, cataracts, and glaucoma.
A diagnosis of diabetic retinopathy can serve as an early warning to patients and doctors about the progression of the diabetes. “In the eye, we are able to see the retinal damage before it causes end organ damage or dysfunction,” observes Dr. Eric D. Hansen, volunteer ophthalmologist with Cure Blindness Project. “The ability to detect retinopathy early is uniquely important because this detection is harder to do—sometimes impossible to do—with other forms of diabetic complications.”
According to Hansen, the damage of the small blood vessels in the eye due to diabetes also occurs in small blood vessels throughout the body, leading to nephropathy in the kidneys, numbness in the legs, and other microvascular damage.
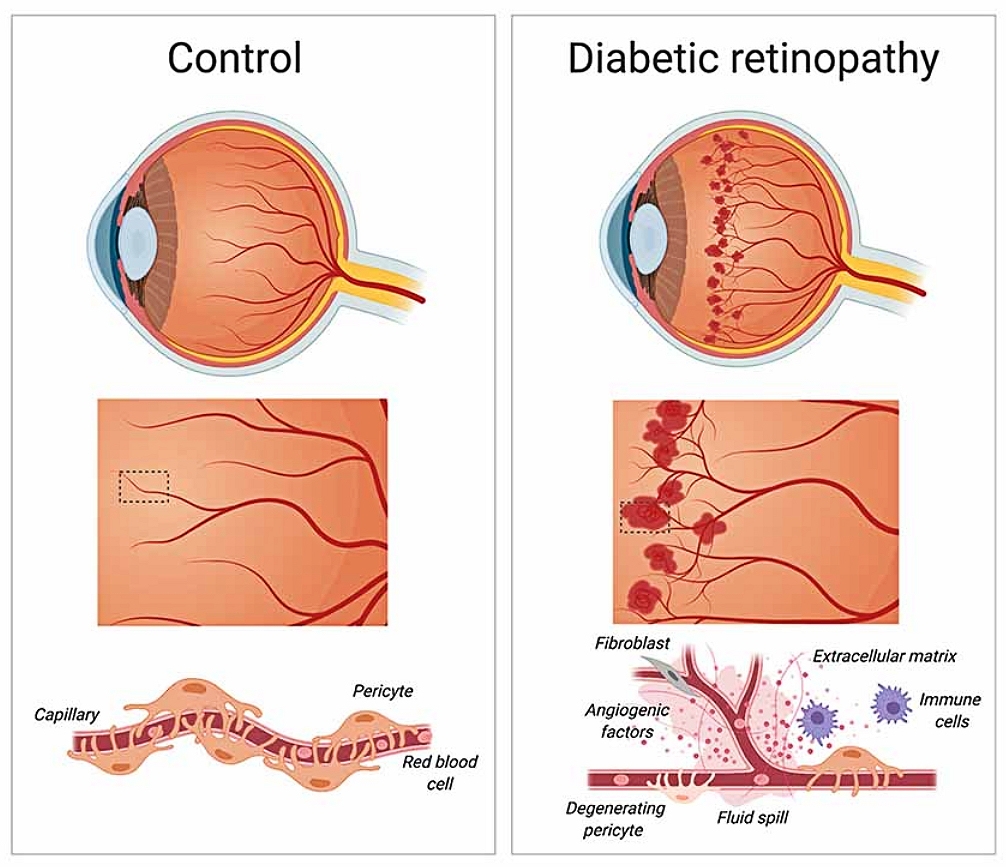
Diabetic retinopathy. During the early stages of diabetic retinopathy, pericytes loss weakens blood capillaries in the retina, causing the formation of microaneurysms, fluid spill and bleeding into the macula. As diabetic retinopathy progresses, the growth of new and irregular blood vessels leads to the formation of scar tissue that causes blurry vision and loss of eyesight. Laredo F, Plebanski J and Tedeschi A. Creative Commons 4.0.
Nonproliferative Diabetic Retinopathy
When the disease is diagnosed early, diabetic retinopathy presents as nonproliferative diabetic retinopathy (NPDR). New blood vessels fail to proliferate (grow), making the retinal vessel walls weaken. https://www.mayoclinic.org/diseases-conditions/diabetic-retinopathy/symptoms-causes/syc-20371611 Vessels dilate, tiny bulges appear, and fluid and blood is released into the retina. https://www.mayoclinic.org/diseases-conditions/diabetic-retinopathy/symptoms-causes/syc-20371611 Sometimes retinal blood vessel damage causes edema in the retina’s macula and, if the swelling decreases vision, treatment is required to prevent permanent vision loss. https://www.mayoclinic.org/diseases-conditions/diabetic-retinopathy/symptoms-causes/syc-20371611
Proliferative Diabetic Retinopathy
Dr. Hansen describes the pathway to blindness from diabetic retinopathy once it reaches the proliferative stage: “The little blood vessels around the retina sustain damage through aneurysms and dilations, leading to abnormal new blood vessels growth (neovascularization), leading to bleeding in the eye and scar tissue (fibrovascular tissue formation), ultimately leading to retinal detachment.”
Vision loss can occur without retinal detachment. Neovascularization can cause a vitreous hemorrhage, which brings with it significant vision loss. Patients only see motions directly in front of the face or have minimal light perception, as the blood obscures the visual input or the light getting to the retina.

Diabetic Retinopathy Causes
What causes diabetic retinopathy? In simplest terms, diabetic retinopathy is related to the blood glucose levels and the dysregulation of blood glucose with diabetic disease.
“Long standing high blood glucose levels cause damage to the blood vessels, to the endothelium, or to the inside of the blood vessels in particular,” notes Hansen.
Blood glucose dysregulation or elevated blood glucose are top risk factors for causing diabetic retinopathy. High blood pressure has a structural impact on blood vessels. There are other forms of retinopathy from hypertension, without diabetes, so the condition can also manifest in isolation.
Any habit or health condition that contributes to high blood pressure is a risk factor for diabetic retinopathy.
Any habit or health condition that contributes to high blood pressure is a risk factor for diabetic retinopathy. Modifiable risk factors include hyperglycemia https://pubmed.ncbi.nlm.nih.gov/11270671/, hypertension, obesity, smoking, and pregnancy. https://pubmed.ncbi.nlm.nih.gov/26676667/ Community struggles such as limited access to healthcare and personal difficulties with health literacy and adherence to therapy also contribute to the progression of diabetic retinopathy.
Non-modifiable risk factors include ethnicity, family history or genetics, age at onset of diabetes, type of diabetes, and duration of diabetes. https://www.thelancet.com/journals/landig/article/PIIS2589-7500(20)30250-8/fulltext
“The risk factors causing vascular disease are synergistic,” Hansen points out. “In general, people who have diabetes have global metabolic disorder, so they have hypertension and high cholesterol or hyperlipidemia. These risk factors work in concert. There's a compounding nature to them.”
Diets Cause Diabetes Worldwide
Early detection gets people into the healthcare system for meaningful intervention. Dr. Eric Hansen
Overeating is commonly linked to diabetes, and Type 2 diabetes with its link to obesity is thought to be a problem in high-income countries like the United States, not in low- and middle-income countries.
This is a misconception, according to Hansen.
“The nature of the diet matters,” explains Hansen, a past international fellow of Himalayan Cataract Project, which later became today’s Cure Blindness Project. ”Although overabundance is missing, poor countries are at risk for metabolic disease because of their dietary narrowness; they have a restrained, carb-dependent diet. Go to Ghana and they are eating lots of corn-based carbohydrates. You go to India and their diet revolves around rice, more starchy carbohydrates.”
Genetic risk factors and shifting diets manifest diabetes across the world, Hansen observes. Low- and middle-income countries are moving away from traditional food sources in favor of higher starch substitutes. “Mixing genetic predisposition with a shifting diet is more likely to cause diabetes in some certain populations,” he notes.
“The foundation of the diet is also over-processed, which comes with the modernization of low- and middle-income countries,” he continues. “This influx of processed foods is highly problematic.”
Diabetic Retinopathy Treatment
When detected early, diabetic retinopathy can be treated through blood glucose control, blood pressure control and health optimization. Early intervention in eye conditions reduces the need for more complex treatments of lasers and surgery. A vision screening that diagnoses diabetic retinopathy can be the first time a patient hears he or she has diabetes.

Dr. Eric Hansen (left) with other trainers and fellows, including Dr. Akwasi Ahmed, after completing a week of retina surgical training with Cure Blindness Project.

Dr. Eric Hansen (left) with other trainers and fellows, including Dr. Akwasi Ahmed, after completing a week of retina surgical training with Cure Blindness Project.
“Early detection gets people into the healthcare system for meaningful intervention,” Hansen says. “We work together with their internal medicine or endocrinologist for metabolic optimization. Ophthalmologists collaborate with the rest of the healthcare system.”
Nariani of Cure Blindness Project describes the process of diagnosing, “We put drops in to dilate the eye. Using a handheld portable device, a direct ophthalmoscope, we look in, see the retina and identify the vessels and the optic nerve to check for glaucoma. We might use the indirect ophthalmoscope—that's a helmet with a headlight that you use with a 20 diopter lens in your hand. By lining up that headlight with the lens on the patient's face in perfect unison, you can detect the full 360 degrees of the retina.” Because it is a retina, back-of-the-eye, posterior segment tool, the indirect ophthalmoscope is also used to identify glaucoma, macular problems, any form of retinal detachment, tears, and/or holes.
More advanced diabetic retinopathy can be treated with intravitreal injections to preserve vision. Intravitreal injections address neovascularization and macular edema. “These are successful at stabilizing the diabetic eye disease, and we can avoid vitreoretinal surgery if we can get those interventions at an optimal time,” Hansen explains. Surgery may be required for advanced stages of the disease.
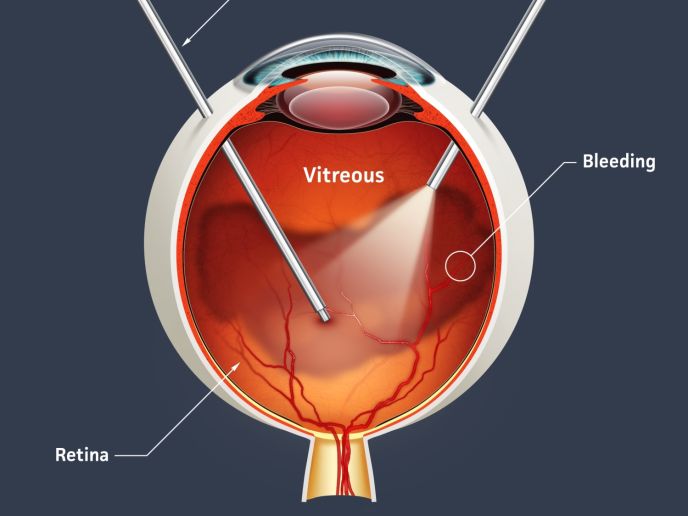
During a vitrectomy, the surgeon enters the vitreous cavity and removes the blood that was caused by abnormal blood vessels.
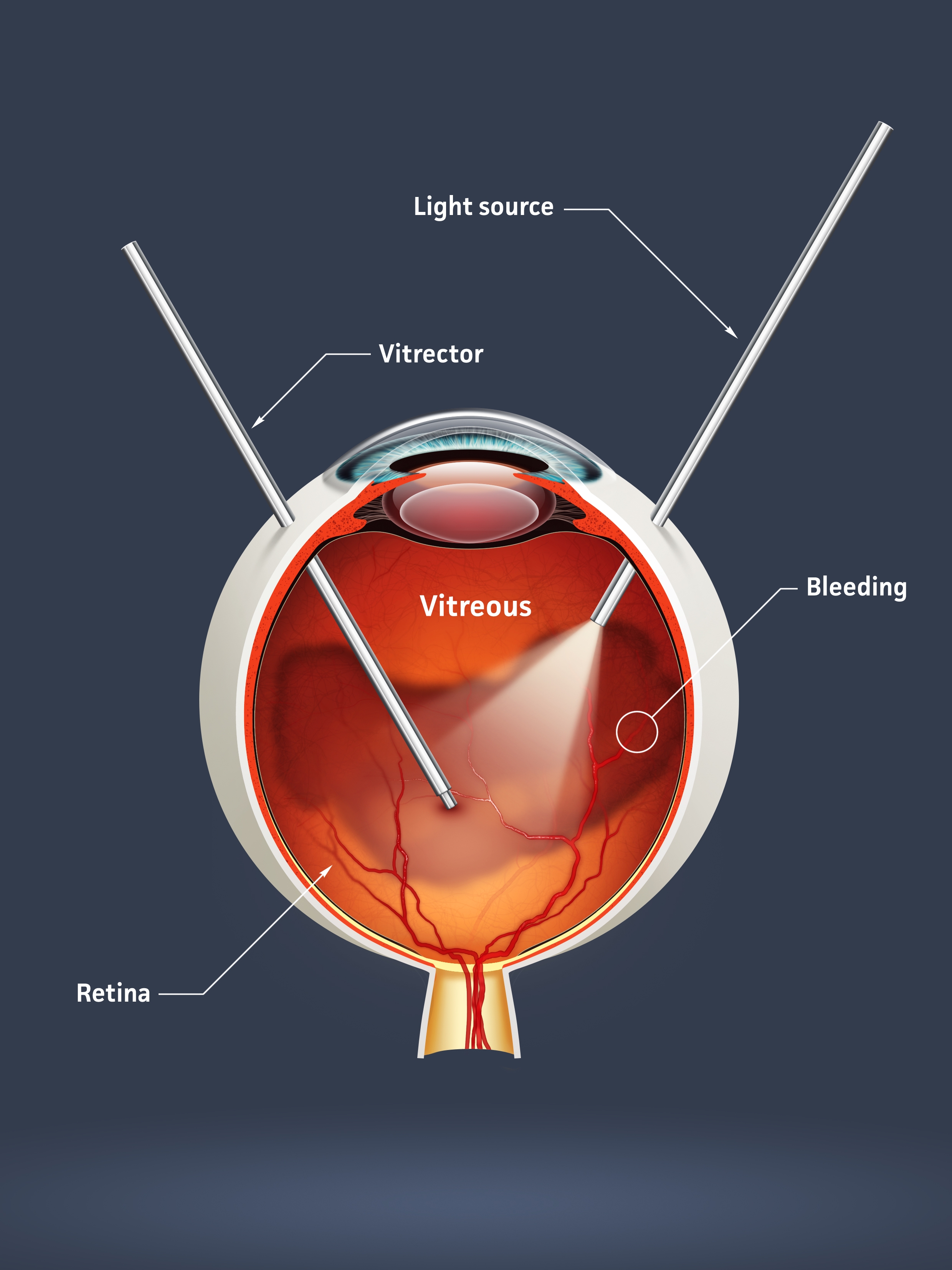
During a vitrectomy, the surgeon enters the vitreous cavity and removes the blood that was caused by abnormal blood vessels.
If the vision loss is caused by abnormal blood vessels, ophthalmic surgeons perform a vitrectomy or a panretinal photocoagulation (PRP). A vitrectomy means the surgeon enters the vitreous cavity and removes the blood. If the vision loss is caused by diabetic retinopathy, a panretinal photocoagulation laser treatment is also performed intraoperatively. A panretinal photocoagulation (PRP) uses lasers to treat retinal ischemia and neovascularization. https://eyewiki.org/Panretinal_Photocoagulation By stabilizing the growth of blood vessels, the procedure also stabilizes the diseased peripheral retina. “This will save or salvage the central vision,” Hansen notes.
If blindness is caused by a detached retina, the goal of ophthalmic surgery is to remove the tractional scar tissue membranes that have developed in order to relieve stretching or pulling on the retina. “We also complete the panretinal photocoagulation, and then [may utilize other needed approaches] including [an intraocular] tamponade—to keep the retina attached and healing,” states Hansen. “This is the approach and reality of a retina surgeon with Cure Blindness Project.”
Difficulties Treating Diabetic Retinopathy in Low and Middle Income Countries
Treatment of diabetic retinopathy—particularly when it involves surgery—in low-and middle-income countries means overcoming challenges: a shortage of surgeons; the high cost of diagnostic and surgical equipment, including consumables; as well as limited access to intravitreal injection treatment.
Countries of Africa face steep shortages of surgical professionals: studies show that, by 2030, six million more surgical care providers will be needed than they are projected to have. https://pubmed.ncbi.nlm.nih.gov/25926323/ Rwanda, for instance, has 162 surgeons when it should have 1,400 to keep up with the surgical needs of its population. The World Health Organization (WHO) recommends a doctor-patient ratio of 1:1000, yet African countries report a scant 0.5 surgeons per 100,000. https://www.msn.com/en-xl/africa/other/how-surgeon-shortage-threatens-lives-across-africa/ar-AA1Af5pc
Hansen describes the retinal surgeries of Cure Blindness Project in a way that makes it clear local training is folded into everything they do with local doctors. “When we're going over there (Ghana), we have an identified timeframe to do hospital-based programming. We provide sub-specialist support, work with our partners, maybe train fellows, give them exposure to different surgical techniques and surgical philosophies, teach a new technique or innovations on techniques, and whatever else is needed.”
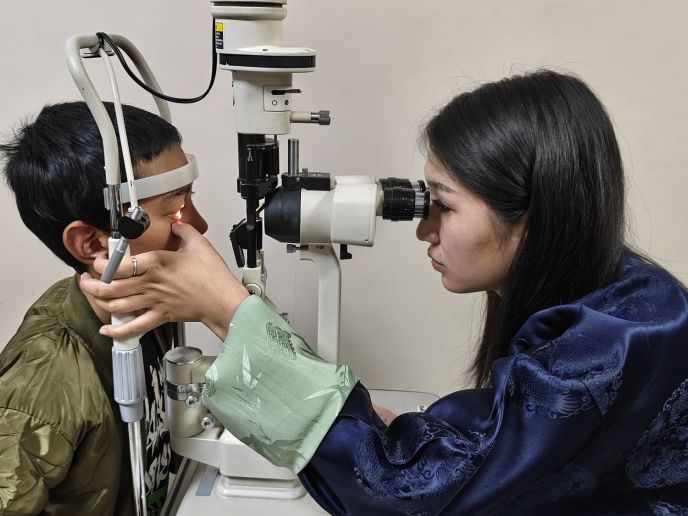
Cure Blindness Project-supported clinical training in Bhutan focused on early detection and management of eye conditions like diabetic retinopathy.
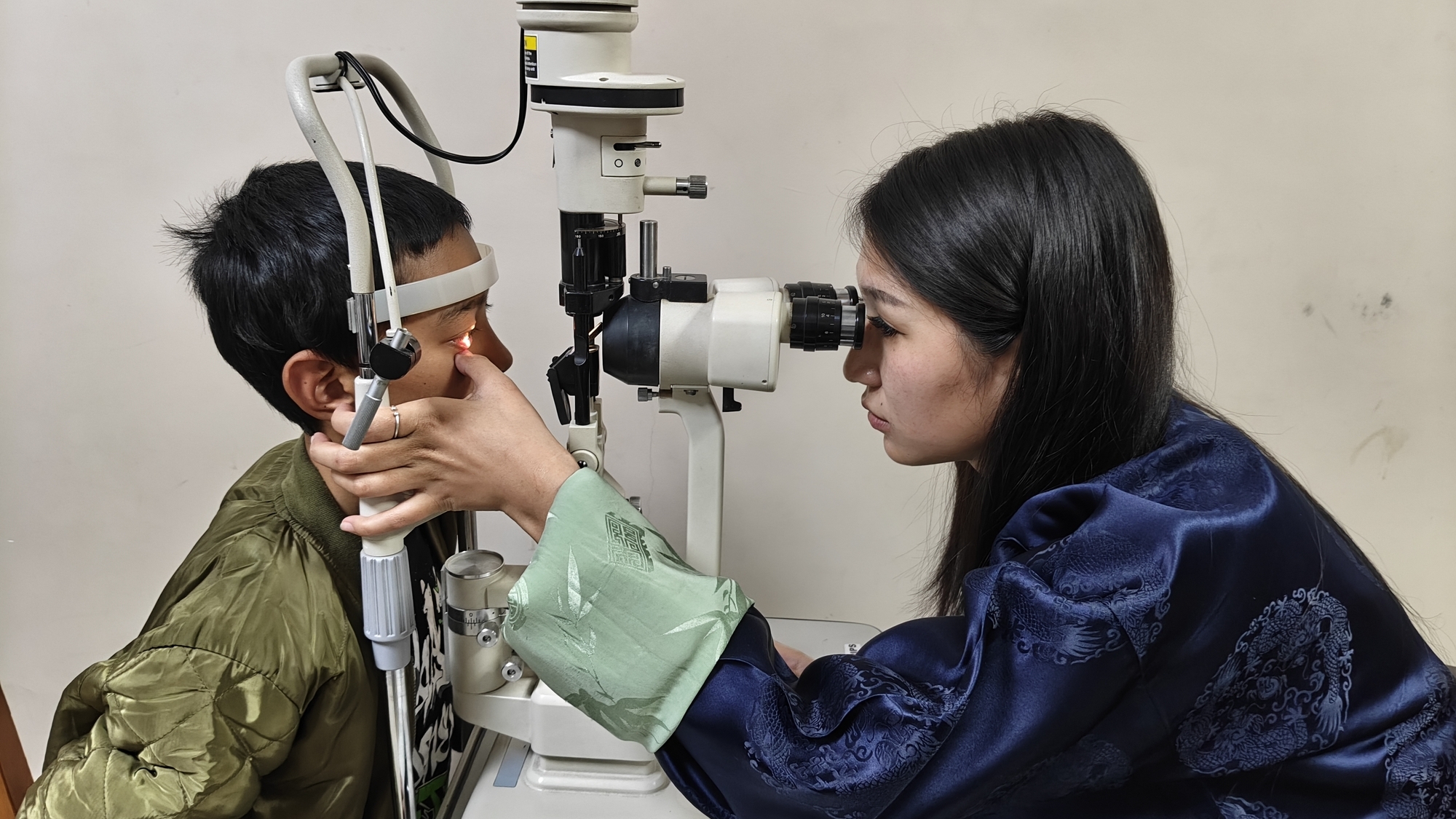
Cure Blindness Project-supported clinical training in Bhutan focused on early detection and management of eye conditions like diabetic retinopathy.
Vitreoretinal surgery requires many consumables. In the United States, retina surgery involves a single-use vitrectomy pack plus consumables. “We open multiple consumables—silicone-tipped aspiration cannulas, forceps, scissors. Each of these are opened individually and then thrown away at the end of the case,” Hansen describes.
The consumables add complexity to the process, putting the surgeries further out of reach for patients in low- and middle-income countries. In many of the places where Cure Blindness Project partners, the government does not provide any reimbursement for retina surgery.
Cure Blindness Project’s partners in India are commendable, according to Hansen. “Their teams have lowered the cost of vitreoretinal surgeries by sterilizing and safely reusing the consumables. It’s really ingenious.”
The challenges of consumables are addressed by Cure Blindness Project too. The organization works with private industry companies like Aurolab, Alcon and Johnson & Johnson to donate important consumables for the hospital-based programs. “We bring hundreds of thousands of supplies that Cure Blindness Project helped procure while also supporting some of our industry friends here in the United States who donated it and let us use it for these philanthropic purposes,” Hansen explains.
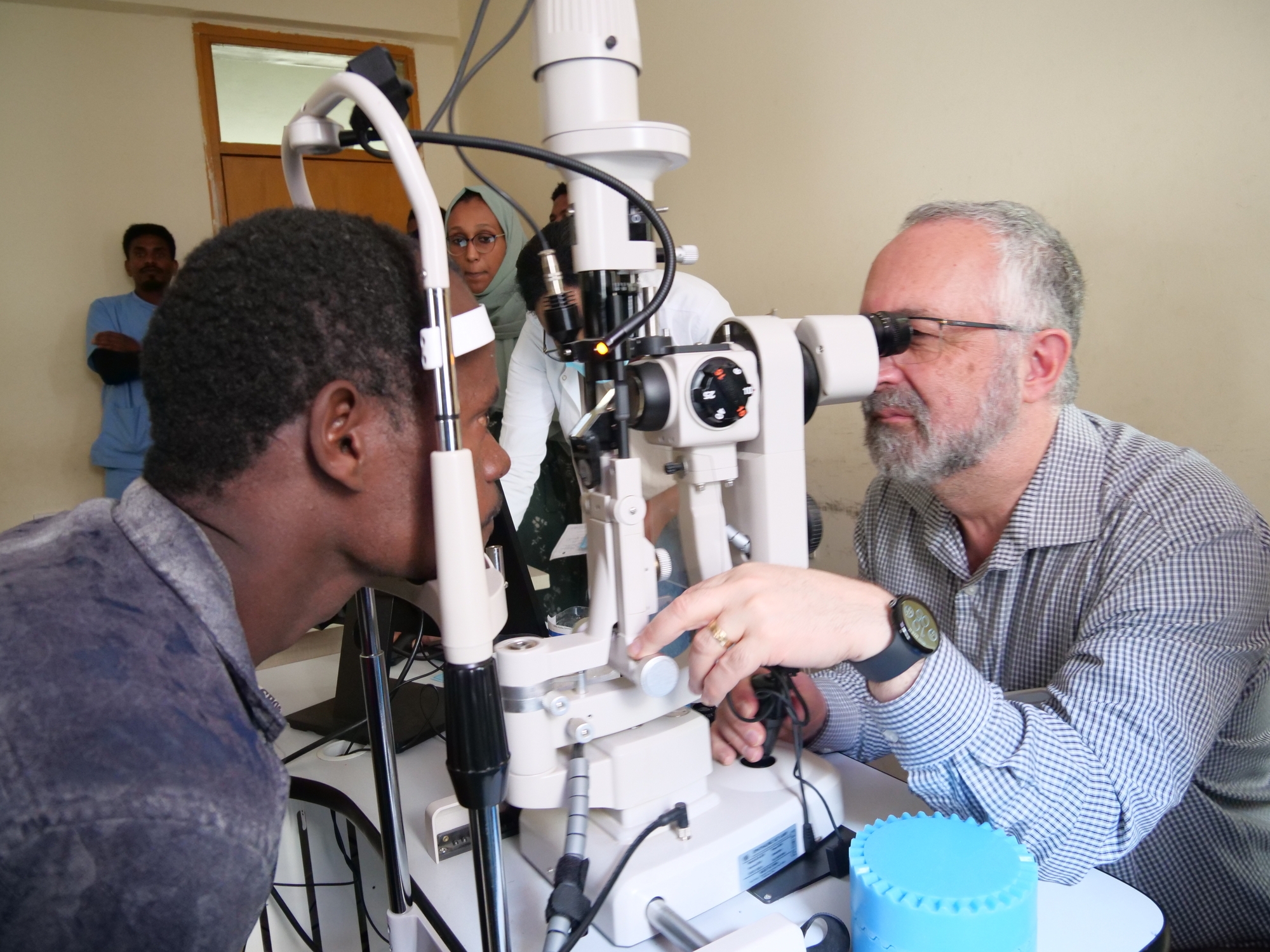
Dr. Paul Bernstein, a key researcher in diabetic retinopathy as well as a clinical advisor of Cure Blindness Project, leads hands-on retina training in Ethiopia.
“By bringing consumables and supplying additional consumables, it alleviates some of that stress or burden on the local hospital,” Hansen states. “Plus we leave everything we bring, so it also becomes this download of additional consumables and packs with everything that they might use in retina surgery.”
How Cure Blindness Project Helps Treat Diabetic Retinopathy
Diabetic retinopathy is a leading cause of blindness in working adults around the world and all of this burden can be drastically reduced. Cure Blindness Project, a global non-profit organization, works on treating diabetic retinopathy and other forms of treatable or preventable blindness in underserved communities in 30 nations across sub-Saharan Africa, South Asia and South America.

Dr. Paul Bernstein, a key researcher in diabetic retinopathy and a member of Cure Blindness Project’s Clinical Advisory Board

Dr. Paul Bernstein, a key researcher in diabetic retinopathy and a member of Cure Blindness Project’s Clinical Advisory Board
Dr. Paul Bernstein, a key researcher in diabetic retinopathy as well as a clinical advisor of Cure Blindness Project, sees the organization’s role as pivotal. “Where we go, we are pioneers in retina procedures,” he notes. “Cure Blindness Project invests in local capacity. We train surgeons in person in their home country and we provide support and mentorship for vitreoretinal fellowships.”
Surgeons like Dr. Akwasi Ahmed from Komfo Anokye Teaching Hospital (KATH) in Ghana.
“The support and mentorship of Cure Blindness Project has allowed me to acquire the skills and training I need to provide the best care possible to my patients,” says Dr. Ahmed of his decades-long relationship with the NGO. Cure Blindness Project has sponsored specialty and sub-specialty training and fellowships including a six-month fellowship at Tilganga Institute of Ophthalmology in Nepal, followed by an intense 12-month fellowship at Aravind in India. “This fellowship makes me one of the few ophthalmologists in Ghana with these skills.”

Dr Akwasi Ahmed, an ophthalmologist, provides training to ophthalmology residents at the Korle Bu Teaching Hospital during the Live Classroom review course organized by Cure Blindness Project and partners in Accra, Ghana.
Today, Ahmed mentors the next generation of ophthalmologists in Ghana, pouring into them as volunteer ophthalmologist of Cure Blindness Project supported and mentored him.
Cure Blindness Project’s model begins with bringing high quality care to those who need it and continues to address diabetic retinopathy through prevention measures and well-trained local capacity. Volunteer ophthalmologists of the organization have performed approximately 1.6 million sight restoring surgeries. For early detection and treatment of diabetic retinopathy and other eye disease, Cure Blindness Project has conducted more than 16.5 million eye screenings and in 2025 sponsored four retina fellowships for ophthalmologists.




